“A powerful tool” for paraplegic patients
A paraplegic injury involves damage to the spinal cord and the nerve pathways running through it. As an important part of the central nervous system, the spinal cord controls various processes in the body, which is why injury may lead not only to paralysis of the extremities, but also to impairments of motor, sensory and vegetative functions. Many affected individuals suffer from spasticity, involving a painful increase in muscle tension or muscle spasms, which further reduces an already diminished level of voluntary movement (consciously controlled motor functions).
Processing of neural signals
The current standard treatment protocol includes physiotherapy and occupational therapy as well as medication. But there is a downside, as Ursula Hofstötter from the Centre for Medical Physics and Biomedical Engineering at the Medical University of Vienna notes: “These drugs do not have a selective effect, meaning that they not only inhibit spasticity, but they also suppress voluntary motor activity and often make people very tired.” Another method that has been found to work well is epidural spinal cord stimulation, which involves stimulating particular nerve structures via implanted electrodes. “In addition to easing pain, this method also has a positive effect on mobility. Patients are able to move parts of the body they were previously unable to move.”
Again, there is a downside as Hofstötter explains: “This is only rarely done, because it requires two surgical procedures and sophisticated technical equipment.” Because of her speciality, one might be inclined to think that Hofstötter is a medical doctor, but in fact she has a background in mathematics. This is how she started to focus on medicine: “A course given by Professor Rattay at the Vienna University of Technology made me aware of neuromodulation techniques. I am very much into sports myself and have had minor accidents that got me thinking: what if I were to lose the ability to walk? This question haunted me and I wanted to bring my knowledge to bear for people who have suffered central nervous system injuries and make a positive difference to their rehabilitation.” – A plan that Hofstötter successfully implemented.
Non-invasive stimulation of the spinal cord
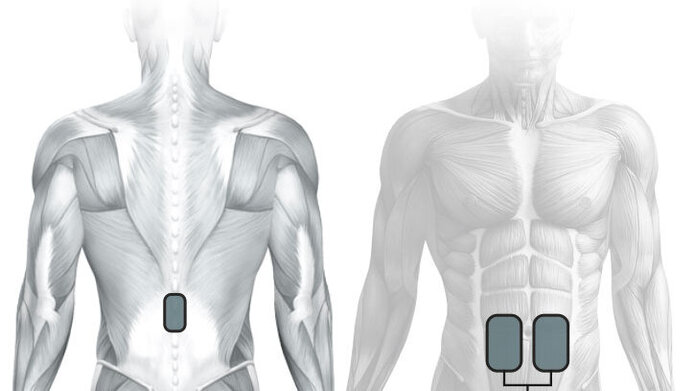
Together with her colleague Karen Minassian, Hofstötter has developed a technique that involves placing adhesive electrodes on the skin and stimulating the same nerve structures as with implanted electrodes. “This is a completely non-invasive method. An added advantage is that it can also be offered by non-specialised rehabilitation centres and clinics.” Studies showed that even a single 30-minute spell of stimulation can successfully control spasticity for several hours and improve residual voluntary motor function. When treatment is continued, the effect can even last for several days.
Making effects more sustainable
In her current FWF-funded project, Hofstötter for the first time focuses specifically on the influence of stimulation on neuronal mechanisms in the spinal cord. “The goal is to be able to offer individually optimised treatment in the future. While there are many clinical studies worldwide, none of them explores the underlying spinal mechanisms. This is the strong point of our research,” says Hofstötter, who heads the research group “Human Motor Control and Neuromodulation” at the Medical University of Vienna. Ten patients with a chronic paraplegic injury (persisting one year after the injury) and 20 people with a healthy spinal cord took part in the study.
Personal details
Ursula Hofstötter is a professor at the Centre for Medical Physics and Biomedical Engineering at the Medical University of Vienna, where she heads the research group “Human Motor Control and Neuromodulation”. Hofstötter received her PhD in technical mathematics from the Vienna University of Technology in 2009. The project “Spinal cord stimulation: sustainable effects on spasticity” (2018–2022) received EUR 191,000 in funding from the Austrian Science Fund FWF.
Reflex arcs for neuronal processes
“The spinal cord comprises a complex neuronal system. We studied several of its mechanisms that we considered as being involved in the development of spasticity both before and after an application of non-invasive spinal cord stimulation.” At this point, it is important to understand the concept of agonist (competitor) and antagonist (opponent): In order to perform a movement, these opposing forces must always interact in a balanced way. If you want to move a joint, for instance, certain muscles must tense and others must remain relaxed. The same goes for the spinal reflex arcs. “We were able to identify various activity-inhibiting mechanisms in paraplegics. After treatment they became similarly active as in people with an undamaged spinal cord. In addition, we were able to identify a mechanism having excess activity that acted in a normalised way after the stimulation treatment.” Data collection is expected to be complete by the end of March.
Patient involvement in research
Carrying out the study successfully required a high degree of interdisciplinary cooperation. “You’re looking at a mix of neurology, physiotherapy, electrical engineering, computer science, physics and, of course, mathematics,” Hofstötter notes and emphasises that the most important cooperation partners are the people affected. “We don’t see them as patients, but as valuable partners on an equal footing. We receive so much information from them that we are permitted to process for research. It is our duty to make the results available for use.” There are already some centres in Vienna that are employing non-invasive spinal cord stimulation in a test phase. If the method proves useful as an individual home therapy, the potential is huge for it to benefit many people in the future. Hofstötter: “There is this misconception that nothing can be done once a condition has become chronic. We absolutely disagree. Spinal cord stimulation is a powerful tool.”
Publications
Hofstoetter, U.S. et al.: Transcutaneous Spinal Cord Stimulation Enhances Walking Performance and Reduces Spasticity in Individuals with Multiple Sclerosis, in: Brain Sciences, 11(4), 2021
Hofstoetter, U.S. et al.: Spinal motor mapping by epidural stimulation of lumbosacral posterior roots in humans, in: iScience, 24(1), 2021
Hofstoetter, U.S. et al.: Transcutaneous Spinal Cord Stimulation Induces Temporary Attenuation of Spasticity in Individuals with Spinal Cord Injury, in: Journal of Neurotrauma, 37(3), 2020