New insights into latent HIV infections
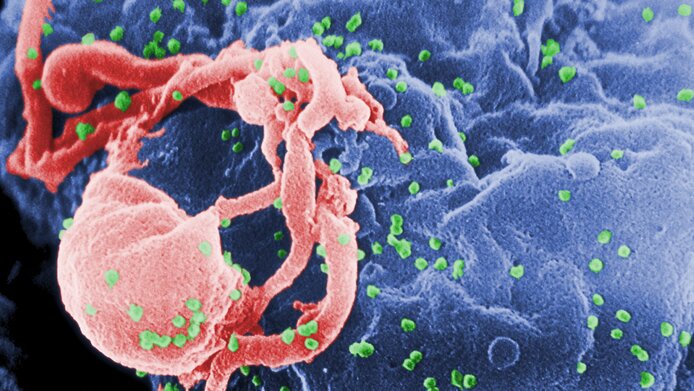
Thanks to modern therapies, HIV infections have become controllable – but these treatments cannot provide a cure. Antiretroviral therapies do indeed manage to keep the number of HI-virus particles in the blood of those infected so low that the outbreak of AIDS is prevented. But the virus cannot be removed entirely. Because it is a master at hiding.
Cellular Hiding Place
One hiding place of the virus that is known are special immune cells called macrophages. The virus can survive inside these cells – beyond the reach of drugs. A team led by Regina Grillari from the Department for Biotechnology at the University of Natural Resources and Life Sciences, Vienna, has found out how the virus can also manipulate the cells to make them more stress-resistant and longer-living. The main focus of the project lay on the enzyme, telomerase, which is active when cells divide and prevents chromosome shortening. Little has been known until now about its activity in cells which, like macrophages, do not divide. The results presented by Grillari were all the more astonishing, as she explains. "We were able to show that the HIV virus induces telomerase activity in macrophages. This was surprising to the extent that the enzyme's known function was connected to cell division which in this case doesn't even take place."
No Function?
A further result showed that telomerase in macrophages does not even pursue its real function – that of lengthening chromosomes – in spite of activation by the HI-virus. Another experiment then supplied clear indications of the role played in this case by telomerase in infected cells. To do so, the reactions of infected and non-infected macrophages to so-called oxidative stress were investigated; oxidative stress is also increased by HIV infections. Results showed that infected cells are able to cope with this stress much better than non-infected ones – and that this is connected to telomerase activation. As Grillari explains: "It seems that the hidden virus particles make their host cells more stress-resistant through telomerase activation, thereby securing their own survival in the long term. A sensible strategy from the perspective of the virus."
"Elite" Research
In another part of the project, so-called "elite" patients were examined. Although these patients are infected with HIV, their bodies manage to so heavily restrict replication of the virus that they can live free of symptoms for years with no therapy. While it is not known how this happens, there are indications that special RNAs (miRNAs) play a role here. Grillari and her team analyzed whether there were differences in the types and frequency of miRNAs circulating in the blood between infected elite patients, "normally" infected and healthy persons. Three different types were indeed identified which occurred in markedly different concentration in the plasma of "elite" patients than in the other groups. Grillari comments: "In future we could use them as biomarkers in order to determine whether people infected are in the 'elite' category or not, and thereby to tailor a therapy to their particular status." The study also succeeded in showing that two of the miRNAs restrict the replication of the virus under laboratory conditions – which means that they could certainly be interesting for new therapeutic approaches. Altogether in this FWF project, Grillari's team succeeded in identifying molecular mechanisms which the HI-virus uses to make macrophages more resistant, thus reprogramming them to become an ideal virus reservoir. At the same time, starting points were found from which it may be possible to combat this reservoir formation with miRNAs.
Personal details Regina Grillari has been conducting research since the mid-90s at the University of Natural Resources and Life Sciences, Vienna, and is currently Professor at the Department of Biotechnology. She is especially interested in exploring and using cell lines for biotechnical applications. She is the co-founder of five biotech companies.
Publications





